When most people in the US think about anthrax, they think about the 2001 terrorist incidents in Washington, D.C., and New York. Melissa Finley (6825) thinks about farmers in developing nations like Afghanistan.
As a researcher in the International Biological Threat Reduction program, Melissa works with veterinary labs in low-resource environments, helping them become safer, more secure, and also more efficient at diagnosing infectious diseases.
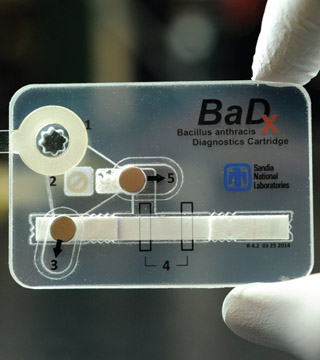
This work inspired the creation of the credit card-sized anthrax detection cartridge, called BaDx, which allows for safer, easier, faster, and cheaper testing for anthrax.
Bacillus anthracis, the bacteria that causes anthrax, is commonly found in soils all over the world and can cause serious, and often fatal, illness in both humans and animals. The bacteria can survive in harsh conditions for decades. In humans, exposure to B. anthracis may occur through skin contact, inhalation of spores, or eating contaminated meat.
Making labs efficient, safer, and more secure
“Working with dangerous samples like B. anthracis spores places laboratory staff at risk. Concentrating many positive test samples in a lab could also tempt someone to steal positive anthrax samples for nefarious uses,” Melissa says.
Currently, samples must be propagated in a laboratory that uses specialized tools requiring a consistent power supply not always available in the developing world, Melissa says.
Then there’s the cost.
“Farmers in many developing countries don’t make a lot of money, so they don’t pay for diagnostic testing often. When they do, they can’t afford to pay a lot for it,” Melissa says.
The most common diagnostic test for anthrax costs around $30, which is out of the reach of many farmers, perhaps discouraging them from testing animals they suspect are infected, Melissa says. The BaDx device, which is more like a pocket-sized laboratory, could cost around $5-$7 and does not require specialized tools to use.
The consequences of not testing animals suspected of having anthrax are life-and-death.
“Because anthracis forms spores when exposed to oxygen, slaughtering or opening the carcass of an infected animal places many people at risk. People can become extremely sick if they come into contact with the spores, either through inhalation or ingestion. The gastrointestinal form of the bacteria can be acquired by eating the contaminated meat,” Melissa says.
Complex and sensitive, but simple to operate
BaDx requires no battery or electric power to operate. It’s hardy against wide temperature variation and can detect very small numbers of B. anthracis spores. That could make it especially useful in parts of the world where anthrax is prevalent, but refrigeration and lab facilities are lacking.
The device can be used by a trained technician in the field. The technician would put a sample swab into the amplification chamber, which contains selective growth media. The device then uses a lateral flow assay, similar to a common pregnancy test, to detect B. anthracis. Magnetically operated valves allow the sample to advance from stage to stage to complete the testing process. If the test is positive for the bacteria, a colored line will appear on the device several hours later.
After testing, the technician can initiate a chemical process that sterilizes the device, which avoids the risk of positive samples accumulating and falling into the wrong hands. In addition to the sterilization process, BaDx is sealed closed, making extraction of live bacteria difficult.
“The device amplifies the B. anthracis so it can detect as few as 100 spores instead of the typical 1 million-10 million required for detection,” says device engineer Jason Harper (8622).
A strong team
Melissa says a strong team of technical staff brought BaDx to life.
Jason and engineer Thayne Edwards (1714) developed the microfluidics platform with the patented magnetic valving that moves the sample through the testing process.
Lead bioscientist Bryan Carson (8622), with technologists Jackie Murton (8622) and Bryce Ricken (8622), developed the selective media formulations, and worked on building and testing the device, as well as helping to develop the decontamination strategy.
Nanotechnology researchers George Bachand (1132) and Amanda Carroll-Portillo (1132) are working on strips for the lateral flow assays.
Bill Arndt (6825), a researcher in the International Biological Threat Reduction program, who works internationally in low-resource environments, provided guidance in device design.
Sandia has licensed BaDx to Aquila, a New Mexico small business that specializes in the design and manufacture of technologies and services for nuclear security and international safeguards.
“We see a lot of potential for government customers and nongovernmental organizations as well as commercial markets,” says Markku Koskelo, chief scientist for Aquila.
The team hopes to use the basic device design to develop tests for other types of disease-carrying bacteria such as salmonella and group A streptococcus, which causes strep throat. Future devices could be created to detect infectious diseases in humans and stem the spread of infectious diseases during epidemics.
The work is funded under Sandia’s Laboratory Directed Research & Development program.
